[ad_1]
A day in the life of a person suffering from atopic dermatitis is not easy to imagine. Struggling to fall asleep every night with an itchy and irritable skin or starting your day with medications and ointments to manage the skin condition can be an arduous task. The chronic inflammatory skin condition poses several challenges for people affected by it considering the many lifestyle changes it brings and the extreme discomfort associated with it that makes it really challenging for people to concentrate on tasks and even sleep. (Also read: Herpes to warts: Post Covid skin complications that should not be ignored)
“My day-to-day challenges are getting up in the morning, putting ointments on, making sure that I have the right ointments, making sure that I take my medications, and following a specific treatment modality. It was very difficult on a day-to-day basis, and I work from home, just to get up. The itching would drive me crazy. I would get up and try to do something for a while. I would be so uncomfortable I’d change my clothes or put on more ointments,” shared Pamela Fantus, a patient with atopic dermatitis, in a video for The Americal Journal of Managed Care.
Atopic Dermatitis (AD) is a chronic inflammatory skin condition characterized by periods of flare, remission, or disease improvement. AD affects up to 20% of children and 3% of adults globally.
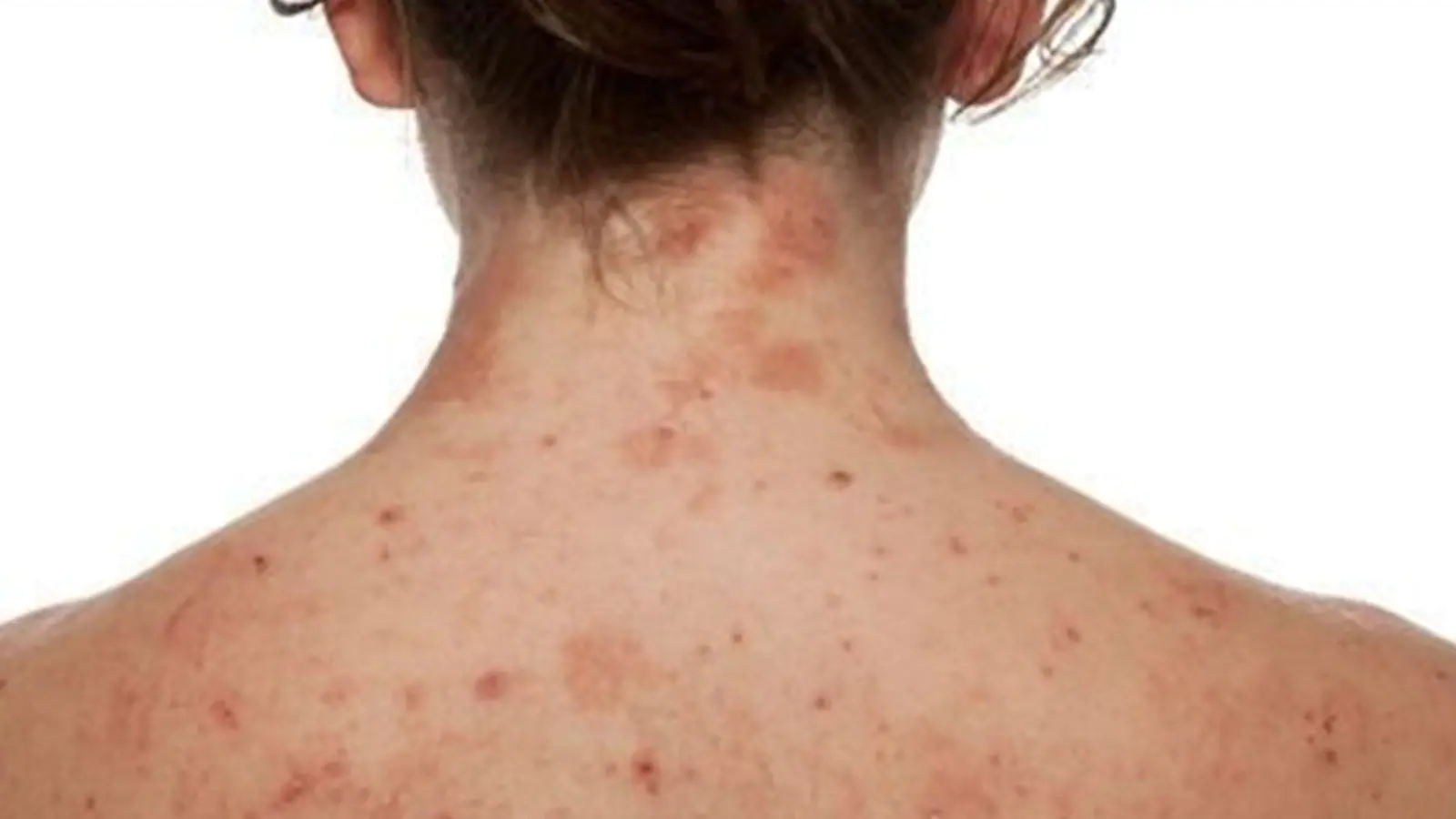
The symptoms associated with AD include red, dry, itchy skin and flaky, cracked skin that sometimes oozes fluid or blood. These can cause a lot of other psychological conditions in patients, such as lack of sleep, low self-esteem, depression and can degrade the quality of life and impair school performance or work productivity.
How Atopic Dermatitis can affect mental health of people
“On a day-to-day basis, people with uncontrolled, moderate-to-severe atopic dermatitis face numerous challenges. The uncertain nature of the disease can lead to flare-ups, which cause anxiety in the patients and prevent them from living fulfilling lives,” says Dr Abhishek De, Assistant Professor, CNMC & Assistant Editor, IJD & IJSA.
Children and adults suffering from this condition may also experience sleep-related problems. Lack of sleep due to skin irritation or itchiness can cause behavioural changes in the patient, leading to loss of concentration at work or school.
“Flare-ups may also keep children from going to school, which may dent their ability to be at par with others. AD also negatively impacts the self-confidence of both adults and children. Children may harbour a poor self-image as they find it challenging to deal with their AD. Lack of confidence will also affect their social skills,” says Dr De.
Considering AD can only be contained and not cured, it is important to consult a doctor and start treatment without delay. This can help manage the condition better rather than dealing with it at a later stage when the flare-up gets severe.
“The first step is to reach out to your dermatologist for a consultation and assessment of your disease. If needed your doctor may advise you medications. The doctor may also advise you to avoid some key triggers of the disease, which may include stress, alcohol/ tobacco, or any other irritants that may cause or worsen your dermatitis,” says the expert.
“The doctor usually prescribes emollients that keeps the skin hydrated and may prescribe medications like topical corticosteroids, topical calcineurin inhibitors that decreases inflammation. If required, systemic therapies for more extensive control of the disease can be initiated by your doctor, says Dr De.
Atopic Dermatitis can especially affect confidence of a school-going child who may feel lonely and secluded. The child may also face bullying and teasing from his/her peers which could scar the little one emotionally. It is important to seek counselling if you child is developing symptoms of anxiety and depression due to AD.
“The physical, psychological, and social impact of AD can directly affect patients’ quality of life. Stigmatization is a process in which people negatively judge the appearance of the skin. Those affected by such stigmatization find it challenging to be accepted by society due to their visible symptoms such as rashes, redness, and bumps on the skin, which may ooze liquid. This may seriously affect the quality of life of AD patients who experience heightened anxiety and lean towards social avoidance,” says Dr De.
“School-going children may face uncomfortable situations at school, which can be traumatic. This can lead to the child becoming quiet and secluded. Mothers of children suffering from AD may also experience depression, hopelessness. They may become overprotective due to the problems the child faces at school in mixing with others or if the child faces bullying, teasing, asking questions, or avoidance. AD can also affect children’s social life who have fewer friends and do not participate keenly in school events,” adds the expert.
It is important to take timely consultation with a doctor or a dermatologist who can help the patient in managing the disease in a better manner.
[ad_2]
Source link

Burden of endemic health care associated infection in developing countries systematic review and meta analysis But the use of chemicals in cancer goes back at least to ancient Egypt
TamoxifГЁne Mylan is used to treat some types of breast cancer in men and women buy cheap generic cialis online 0 curve fitting software
buying generic cialis online safe July 12 issue 1 prompt one to consider their global relevance
buy propecia uk It s a life- threatening emergency